Do I have Irritable Bowel Syndrome or Inflammatory Bowel Disease?

Do I Have Irritable Bowel Syndrome (IBS) or Inflammatory Bowel Disease (IBD)?

I don’t know about you, but if I mention Inflammatory Bowel Disease (IBD), I frequently get the response “oh yes, my friend has that.”
After a bit of digging, it is clear that they are confusing IBD with Irritable Bowel Syndrome (IBS). Do you run into this same scenario when trying to explain your diagnosis (or the diagnosis of your child) to someone else?
While IBS and IBD can share symptoms, they are two very different conditions in etiology and in terms of management.

Inflammatory Bowel Disease refers to an autoimmune disease with inflammation of the gastrointestinal (GI) tract. IBS, on the other hand, is a functional GI disorder that may cause similar symptoms but without damaging the GI tract.
According to the International Foundation for Gastrointestinal Disorders, “IBS is the most common functional disorder diagnosed by gastroenterologists and accounts for up to 12% of total visits to primary care providers.” Functional disorders are conditions where there is an absence of structural or biochemical abnormalities on common diagnostic tests.
Determining the correct diagnosis when it comes to IBD vs IBS is crucial. Each has its own distinct treatment path, but similar early symptoms can confuse both healthcare providers and patients alike.
Read on to learn more about the types of IBD and how nutrition plays a crucial role along the path of diagnosis and treatment.
Two Types of Inflammatory Bowel Disease
Presently, IBD is most commonly categorized as either Crohn’s disease or Ulcerative colitis (UC). There is likely a wide range of in-between cases for these diagnoses, but for now, this is how we differentiate the two types. The images below can help to answer common questions about the two types of this condition.
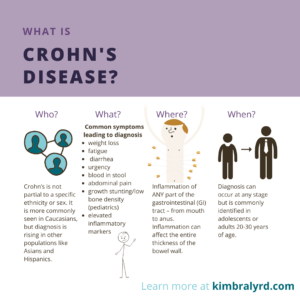
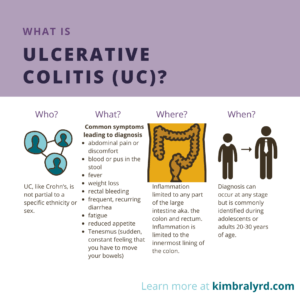
How Common Are IBS and IBD?
According to the International Foundation for Gastrointestinal Disorders (IFFGD), IBS is “the most common functional gastrointestinal (GI) disorder with worldwide prevalence rates ranging generally in the area of 10-15%.”
Currently, it is estimated that as many as 3.1 million Americans are affected by IBD, and many are diagnosed before the age of 35.
Shared Symptoms of IBS and IBD
IBS and IBD share some symptoms and similar demographics of patients (2). A recent study found that 73% of IBD patients (UC + CD) whose colonoscopy and bowel tissue exams showed their disease was in remission still met the diagnostic criteria for IBS. Researchers found the 29% of IBD patients in remission were mis-categorized as flaring due to IBS symptoms (3).

The bottom line about the relationship of IBS and IBD from the current research is that the two share commonalities and patients with IBD are more likely to suffer from IBS-like symptoms (3). However, other associations have not been made clear or supported by evidence.
Both IBS and IBD can have a significant impact on quality of life and day to day management. Two doctors did an excellent job of summarizing the issue of confusing the two conditions when responding to a recent study in a letter to the editor of Clinical Gastroenterology and Hepatology (4):
“…we believe that caution is needed before attributing persistence of symptoms in patients with IBD in remission to IBS…we agree that a better understanding of the frequency of IBS in patients with IBD is needed, especially as it relates to the patient’s psychological health…In addition, heightened awareness of these…ongoing symptoms is needed whenever a patient with IBD and…markers of inflammation is seen so as to not misclassify them as having IBS-type symptoms.”
Patients with IBD during the long-standing remission phase tend to present commonly with IBS-like symptoms and quality of life seems reduced in patients with such symptoms (5). More research is needed to pinpoint the percentage of IBD patients in demonstrated remission that then meet diagnostic criteria for IBS.
IBS vs IBD: Which Do I Have?
In most cases, a combination of the following findings will help tell the difference from IBD vs IBS:
- Your signs & symptoms
- Your laboratory test results
- Your imaging results
- Your endoscopy and biopsy results
IBD patients often have IBS-type symptoms, and this can complicate your path to a clear diagnosis, especially given how commonly IBS is diagnosed. It is important to persist until you have a proper diagnosis because IBS and IBD require different treatments (2).
FAQs About IBS and IBD
1. Can IBS cause back pain?
Yes, back pain is relatively common among most IBS patients, although we don’t know exactly why. Similarly, researchers estimate that up to 25% of IBD patients also experience chronic back pain.
2. Can IBS cause weight loss?
IBS can result in significant weight loss, especially when patients experience abdominal cramping and pain that causes them to eat less frequently. Those with IBD may also lose weight due to diarrhea, inflammatory issues, and increased energy consumption rates.
3. Can IBS cause weight gain?
On the flip side, IBS can also cause weight fluctuations and gains, especially if the patient deals with constipation and bloating. IBS is even more likely to lead to weight gain in many individuals.
4. Can IBS cause fatigue or make you tired?
Yes. As many as half of the patients with IBS or IBD report feeling fatigued, exhausted, or tired. This can be caused by bowel-related symptoms, but also by the psychological distress of the two diseases.
5. Will IBD go away on its own?
No. IBD cannot be cured, although patients can enter periods of remission in which the disease is not active. IBS, on the other hand, is not necessarily permanent. The condition can be treated and go away over time, although many cases do reappear.
6. How can I deal with IBS constipation?
IBD constipation is a common complaint and one that can be difficult to treat. Some of the best management tactics include drinking more water, exercising enough, and eating more fiber.
Speaking of diet changes, we need to talk about dietary therapy and IBS/IBD.
What Does Nutrition Have to Do With IBD and IBS?
A proper diagnosis plays a pivotal role in treatment. Food-related quality of life depends on the following factors:
- The impact of the diet
- Eating behaviors
- Food related anxiety
A study evaluating the factors listed above in patients with IBD and IBS found that both patient groups follow various diet treatments either on their own or directed by a dietitian (less common).
Both IBD and IBS patients with more severe symptoms and on multiple elimination diets reported poorer food-related quality of life. In this study, patients in both groups were more likely to self select a diet rather than follow a medically prescribed diet.
Overall, patients with IBS followed dietary treatment more often than those with IBD. These results along with a growing collection of research report that food is a powerful tool in disease management and patients frequently follow dietary modifications without guidance. This in turn may lead to unnecessary eliminations, frustration and decreased quality of life.
Professional education on IBS and IBD nutrition from a GI dietitian is essential for symptom management and alleviation. More studies, as always, are needed particularly in the area of food-related quality of life.
Studies do show that a multidisciplinary team can help with treatment options, mental health, quality of life, care coordination and other crucial factors. Assistance should extend throughout the course of the disease, including during diagnosis, treatment, and into management and maintenance stages. This can ultimately improve daily quality of life, with food being an integral part (6).
The Power of Obtaining the Right Diagnosis
A correct diagnosis and treatment plan can make all the difference in the quality of life for someone with a GI disorder. For both conditions, dietary therapy is best supported by a multidisciplinary team including GI doctor, trained dietitian, and psychologist.
A multidisciplinary team is crucial along the path of diagnosis, treatment, and recovery. The image below illustrates an ideal composition of healthcare teams for both conditions:

IBS and IBD Treatment Options
Treatment options differ according to diagnosis. For IBS, the primary treatment is a combination of managing diet, lifestyle, and stress, with or without medication and counseling. Treatment for IBD first must address treating the inflammation which is life-long.
For both IBS and IBD, tailored diet Interventions are a key component of treatment and maintaining quality of life.
While there are no cures currently available, treatments such as medications, surgery and nutrition therapies focus on eliminating inflammation and managing symptoms. Untreated IBD can wreak havoc and lead to complications down the road. Therefore, treatment of this disease is essential for life.
Effective treatment can have a profound impact by healing the GI tract from chronic inflammation and damage and improving quality of life. IBS in contrast can often be managed by diet and lifestyle and does not cause changes in bowel tissue.
Does Every IBS or IBD Patient Respond to Dietary Therapy?
In a nutshell, dietary therapy for IBD is a way of alleviating symptoms and inducing remission using specific nutrient-dense foods and excluding certain other foods. There are an increasing number of different dietary therapies with growing bodies of research to support them.
While we haven’t proven exactly why they work, the evidence suggests that they do work for many patients alone or in conjunction with their medication plan.
Similarly, a recent study reported that the majority of the IBS providers surveyed recommended diet therapies to their patients. Among the most commonly recommended interventions for IBS are the inclusion of
- Lactose-reduced foods
- Gluten-free foods
- Low fermentable oligosaccharides, disaccharides, monosaccharides, and polyols (FODMAP)
- High-fiber foods
- Low-fat diets
Unfortunately, a minority of GI providers refer their IBS patients to a registered dietitian for nutrition counseling, and of those who are referred, few are referred to dietitians with specialized GI training (7).
For many individuals, IBS and IBD nutrition therapy is a critical piece of a treatment protocol that may also involve medication. For others, dietary therapy can work on its own. For some, dietary therapy may not work as part of their therapy regimen.
For both IBS and IBD, and no matter the treatment plan, it is important to have a specialized healthcare team focused on the individual, condition, and improving their quality of life. With a great team and a clear dietary plan, remission and recovery can be possible.

Want to Learn More About IBD vs IBS?
In need of diet support for inflammatory bowel disease? Visit my diet therapy resources to learn more about nutrition support and how it can help you.
References
- Crohn’s & Colitis Foundation. Inflammatory Bowel Disease vs. Irritable Bowel Syndrome. DiaSorin S.p.A. 2019. Accessed at https://www.crohnscolitisfoundation.org/sites/default/files/2019-10/ibd-and-IBS-brochure-final.pdf.
- Quigley EM. Overlapping irritable bowel syndrome and inflammatory bowel disease: less to this than meets the eye?. Therap Adv Gastroenterol. 2016;9(2):199-212. doi:10.1177/1756283X15621230
- Perera LP, Radigan M, Guilday C, et al. Presence of Irritable Bowel Syndrome Symptoms in Quiescent Inflammatory Bowel Disease Is Associated with High Rate of Anxiety and Depression. Dig Dis Sci. 2019;64(7):1923-1928. doi:10.1007/s10620-019-05488-8
- Hirten R, Colombel JF. Need for Caution in Diagnosis of Irritable Bowel Syndrome in Patients With Inflammatory Bowel Disease. Clin Gastroenterol Hepatol. 2017;15(8):1315. doi:10.1016/j.cgh.2017.04.008
- Ozer M, Bengi G, Colak R, Cengiz O, Akpinar H. Prevalence of irritable bowel syndrome-like symptoms using Rome IV criteria in patients with inactive inflammatory bowel disease and relation with quality of life. Medicine (Baltimore). 2020;99(19):e20067. doi:10.1097/MD.0000000000020067
- Guadagnoli L, Mutlu EA, Doerfler B, Ibrahim A, Brenner D, Taft TH. Food-related quality of life in patients with inflammatory bowel disease and irritable bowel syndrome. Qual Life Res. 2019;28(8):2195-2205. doi:10.1007/s11136-019-02170-4
- Lenhart A, Ferch C, Shaw M, Chey WD. Use of Dietary Management in Irritable Bowel Syndrome: Results of a Survey of Over 1500 United States Gastroenterologists. Journal of Neurogastroenterology and Motility. 2018;24(3):437-451. https://doi.org/10.5056/jnm17116

Hi! I'm Kim Braly, RD, a clinical researcher and IBD Nutrition Consultant. I specialize in cutting-edge dietary therapies for inflammatory bowel disease that have been shown in multicenter trials to decrease inflammation, alleviate IBD symptoms and induce remission. I'm passionate about offering this effective new option to patients and their families with my 3D-Dietary™ Approach for IBD and helping to usher in a new era of IBD treatment through mentoring and research trial consultation. Let's see what diet can do for you.
ABOUT
FOR PATIENTS

Flares Happen!
You can't always put your life on hold when IBD rears its head, but you can make this your easiest flare yet. My proven diet and lifestyle tips support your gut, body, mind & emotions for a faster recovery and a longer remission.
FOR PARENTS

Is Your Child’s Weight Dropping Fast?
You don't have to stand helpless during an IBD flare. Feed your child foods proven to minimize triggers, calm inflammation, and repair the gut. Get them healing and growing!




