Dietary Fats in Crohn’s, Colitis and IBD: What the Research Suggests You Should Eat

We all get mixed messages about fats. We’re told they’re harmful and should be limited. But then we hear there can be “good” fats and “bad” fats. With IBD, it gets even more confusing. Have you had a well-intentioned doctor tell you to limit or avoid fats for your Crohn’s or Ulcerative colitis?
In this article, you’ll learn about types of fats, their purpose, and what the most up-to-date scientific literature suggests about dietary fat for those with UC, Crohn’s or Inflammatory Bowel Disease (IBD) in general.
I’ve also included my evidence-based Fat Guide Pyramid to use as a reference for your professional practice or personal life, since studies aren’t always available on this topic.
What is Dietary Fat?
Dietary fat is one of the three main macronutrients (along with carbohydrates and protein). Macronutrients are nutrients in the diet required in larger amounts, as opposed to micronutrients (vitamins and minerals) needed in smaller quantities.
Fats, sometimes called lipids, have a different chemical structure than proteins and carbohydrates (carbs). This means that the body digests fats in a different way than it does proteins and carbs.
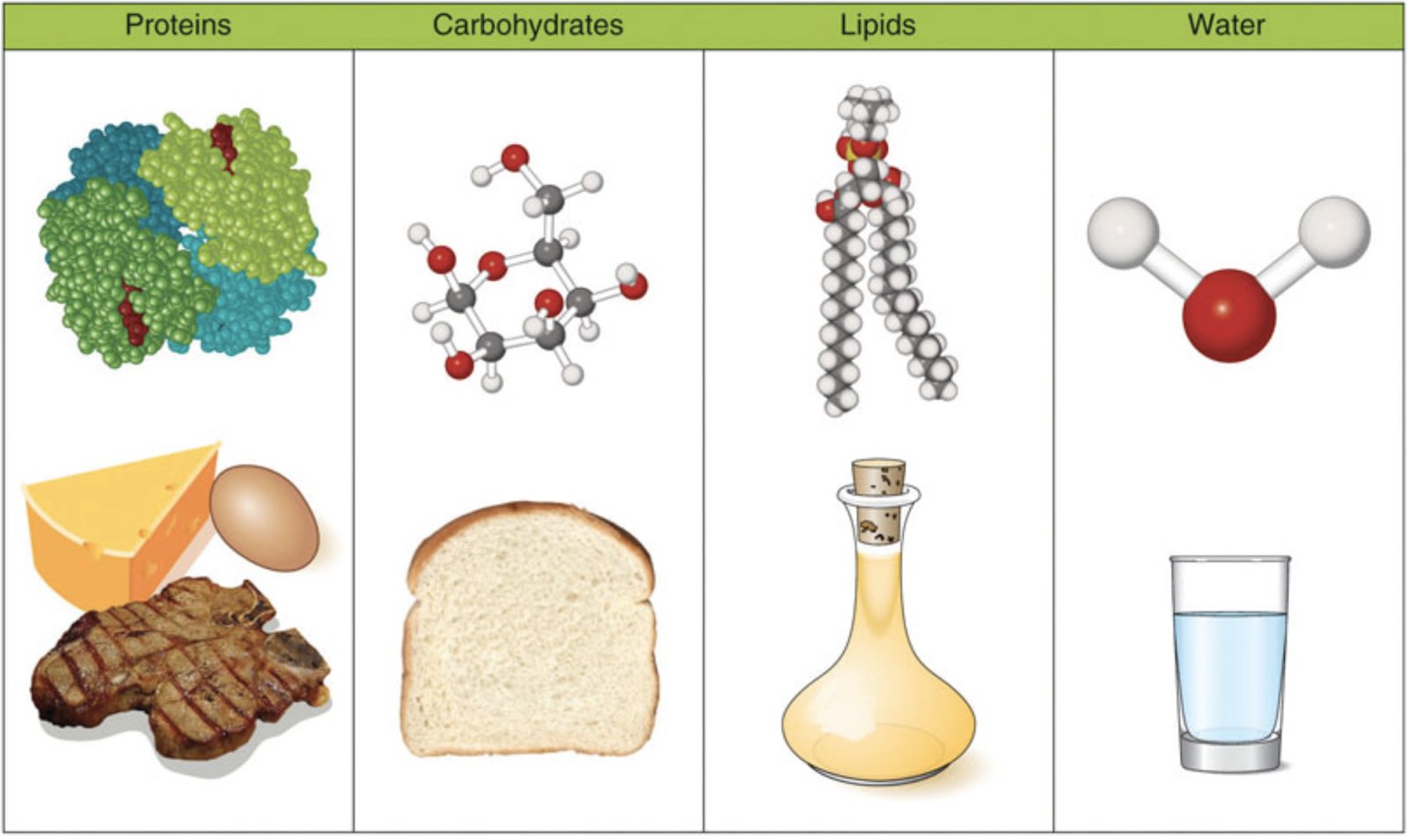
Image courtesy of Open Oregon Educational Resources.
Why Is Fat Important?
Recall the 80’s and 90s when fats were villainized and people started to think of fat as “bad.” Some even cut them out entirely from their diet and replaced full-fat options with “fat-free” or “low-fat.” The problem is, foods don’t taste or feel as good without fat. Manufacturers responded by using extra sugar and all sorts of additives in our food supply to compensate for the missing fat.
We now know this was a misguided trend. Dietary fats are part of a well balanced diet and are NECESSARY for normal functioning in the body. Without them humans can experience growth stunting and vitamin deficiencies. This means fats are especially critical in children’s diets.
Fats help with vitamin absorption and cell membrane creation, and play a role in hormone production. They help regulate blood sugar and mitigate food cravings by promoting satiety (a feeling of fullness).
Current recommendations for an individual suggest 20 to 35% of overall energy intake each day should come from fats. I have analyzed hundreds and hundreds of food logs for pediatric and adult patients with IBD. While there isn’t current evidence to support this, in my experience, some individuals with IBD may need even more fat to prevent or minimize weight loss during times of inflammation or when catch up growth/weight gain is indicated.
For both adults and children, nutrition-rich fats are a key part of making IBD nutrition plans and diets, like the Specific Carbohydrate Diet (SCD), sustainable and satisfying.
The Link Between a Western Diet and the Development of IBD
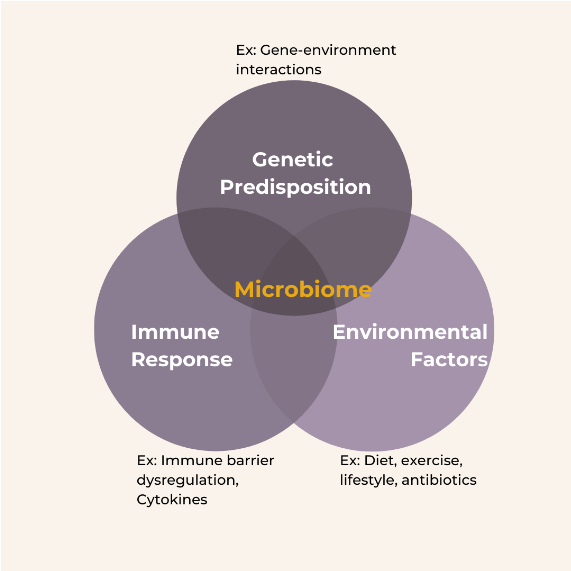
Specific, long-term dietary patterns are linked to the development of IBD in industrialized countries. These patterns include:
- ⇩ intake of soluble and insoluble forms of fiber
- ⇩ intake of fruits and vegetables
- ⇧ intake of sugar
- ⇧ intake of refined carbs
- ⇧ intake of processed foods & food additives
- ⇧ intake of red and processed meats
- Imbalanced ratio of polyunsaturated fatty acids Omega (n)-3 and Omega (n)-6 fatty acids in the diet
Cholesterol, Saturated & Unsaturated Fatty Acids (FAs)
Cholesterol
Cholesterol is a type of fat. It is found in your blood and comes from two sources:
- Dietary intake– from animal products such as meat, dairy and eggs
- The liver– which makes cholesterol for your body and adjusts production based on circulating levels.
A certain level of cholesterol is needed to keep the body functioning normally. There are two main types:
- Low density lipoprotein (LDL) serves an important role as the carrier of cholesterol to tissues in the body where it is used for creating cell membranes or is converted to hormones. High blood levels of LDL over time is a risk factor for cardiovascular disease. For this reason it is commonly referred to as “bad” cholesterol.
- High density lipoprotein (HDL) removes excess cholesterol from cells. It has been suggested recently that HDL may play an anti-inflammatory role. So, LDL and HDL work in tandem and higher levels of HDL are good. Factors such as weight, exercise and diet impact HDL levels. HDL is commonly referred to as “good” cholesterol.
Saturated Fats
In addition to HDL cholesterol, saturated fatty acids (SFAs) can also have a negative effect on health if consumed in excess. SFAs are primarily found in animal foods and some plant sources (i.e. palm kernel and coconut oils). Saturated fats are considered neutral (not “good” nor “bad”), but a diet high in saturated fat intake over time can promote high levels of LDL and lead to inflammation. In studies on mice, saturated fat intake is also associated with more IBD flares.
Unsaturated Fatty Acids
Unsaturated fatty acids (UFAs) are broken down into two groups.
1. Monounsaturated fatty acids (MUFAs) – found in plant-based oils such as olive, canola, peanut, safflower and sesame as well as various nuts and avocado.
⭐ Research has shown that dietary patterns high in olive oil, such as the Mediterranean and the Crohn’s Disease Exclusion Diet (CDED) may have a positive or protective effect on intestinal inflammation.
2. Polyunsaturated fatty acids (PUFAs) – include both n-3 (omega 3) or n-6 (omega 6) fatty acids. These fatty acids are essential as they cannot be made in the body and must be obtained from food sources.
N-3 fatty acids are found in:
- Fatty ocean fish such as salmon, mackerel, and herring
- Seeds and nuts (Ex: flax, hemp, chia and walnut).
N-6 fatty acids are found in:
- Most plant oils (Ex: flax, soy and canola)
- Meat and poultry fat, from animals fed grain-based feed
N-6 fatty acids from plants and meat account for ~90% of the fatty acid intake in the typical U.S. diet.
⭐ Meat and poultry fed on grain-based feed has a higher ratio of n-6 to n-3 fatty acids than meat sources that are grass-fed. In other words, grass fed meats show a higher concentration of n-3 fatty acids. Similarly, the fatty acid composition of farm-raised salmon fed with plant sources (Ex: corn, or soybean meal) vs. wild caught salmon shows a higher concentration of n-6 fatty acids.
From the research that has been done, we know that the typical American diet contains nearly 11-30 times more n-6 than n-3 fatty acids. This is thought to be one of the major contributors to the rising rate of inflammatory disorders, with a higher ratio of n-6 to n-3 promoting higher levels of inflammation.
What Do Studies and Expert Guidelines Say About Fats and IBD?
Guidelines published in 2021 from the International Organization for the Study of Inflammatory Bowel Disease (IOIBD) concluded that for those with UC:
⭐ It is prudent to reduce intake of Myristic Acid (a long-chain saturated fat found in palm/coconut oils and dairy fats from meat from GRAIN-FED vs GRASS-FED animals).
⭐ The authors found while evidence is weak overall, foods naturally high in n-3 and low in n-6 may be beneficial.
⭐ The evidence is inconclusive as to whether supplementation of n-3 from fish oil has the same positive impact as fish oil from foods.
In a recent cross-over study published in the Journal of Clinical Gastroenterology and Hepatology, researchers examined the relationship between dietary fat and colonic inflammation in IBD patients with inactive UC as well as quality of life (QOL). Participants were randomized into two diet arms for four weeks that received catered meals for either a low-fat, high fiber diet (LFD, 10% kcals from fat, n-6:3 ratio of ~3:1) or an improved standard American diet (iSAD, 35-45% kcals from fat, n-6:3 ratio of ~25:1) which included higher quantities of fruits, vegetables and fiber than a typical Standard American Diet. Participants then switched diet arms for another 4 weeks. The study was controlled for other lifestyle changes such as increased physical activity.
Results of this study showed that both a LFD and iSAD produced an increased quality of life. The low-fat, high-fiber diet decreased markers of inflammation and reduced intestinal dysbiosis in fecal samples compared to participants’ baseline/Standard American Diet. While the sample size was small, researchers concluded that dietary interventions might benefit patients with UC in remission.
With both diets, the following changes occurred from participants’ baseline:
- ⇧ intake of fruit servings
- ⇧ intake of vegetable servings
- Improved ratio of n-6:3 fatty acid intake
- ⇩ intake of red meat
- ⇩ intake of sugar
- ⇩ intake of total fat
My Take on n-6 and n-3 Fatty Acids and IBD
Many of the research studies on n-6 vs n-3 fatty acids in the diet, and most done on the IBD population, do not specify grain-fed vs. grass-fed beef, grain-fed vs. free range chickens or farm-raised vs. wild fatty fish. This makes it difficult to draw clear conclusions. However, given the evidence that higher n-6 to n-3 ratios are associated with increased inflammation and that grass-fed meat and poultry have improved ratios, it may be appropriate for those with IBD to prioritize grass-fed and free range protein sources when possible.
If you are looking for where to find grass-fed/pasture-raised options, first, look for local options around you such as cow or pork shares. Resources like US Wellness Meats or Butcher Box are great online options that will deliver to you.
Here are the links to my Organic, Grass Fed, and Free Range series for more information on this topic:
- Organic, Grass Fed, and Free Range: What do they mean? (Part 1 of 3)
- Organic, Grass Fed, and Free Range: Nutrient Quality & Health Benefits (Part 2 of 3)
- Organic, Grass Fed, and Free Range: Label Deciphering and Take Home Resources (Part 3 of 3)
Discussion on Red and Processed Meats:
⭐ The IOIBD guidelines also suggest reducing intake of red and processed meat in UC based on some evidence associating red meat intake with worsening UC.
⭐ For CD, the authors found it was unnecessary to restrict moderate consumption of unprocessed red meat, lean chicken meat, and eggs. They did not define what moderate consumption is. Recent clinical trials showed that a diet with mandatory, daily intake of chicken breast and 2 eggs was associated with high rates of remission in both children and adults with Crohn’s Disease.
I will note that red meat and processed meats are frequently grouped together in the literature and diets of the individuals are not discussed in great detail. The studies that have been conducted suggest that diets high in red meat or processed meats tend to also be diets with lower consumption of MUFAs and PUFAs, legumes, fruits, and vegetables.
This means we can presume that those who consume a diet high in red and processed meats also consumed LESS whole foods given the dietary trends of industrialized countries noted above.
I have yet to find an article that discusses what type of meat study participants consumed (i.e. grain-fed vs. grass-fed) or one that separates red meat from processed meat. Processed meats contain sulfur-containing amino acids found in additives and preservatives that are linked to increased risk of inflammation and colon cancer.
My conclusion is that it’s still unclear whether grass-fed red meat should always be excluded from the diet of those with IBD, but individuals may choose to avoid all red meat out of caution, or for various other personal reasons.
What about Trans Fats and Hydrogenated Oils?
There are some fats that have no health benefit, namely trans fats. Trans fats are primarily created through hydrogenation (processing to stabilize oils in our food system). Trans fats are found primarily in processed and fried foods, frequently from restaurants. Due to health concerns, their abundance in the food supply has significantly decreased.
Recommendations for IBD & Trans Fats:
According to the IOIBD guidelines, long-term intake of trans fats in a prospective study was linked to increased incidence of UC.
⭐ It is recommended to avoid trans fats in both UC and CD.
Dairy & Animal Byproducts
Animal byproducts, which include the following types of foods, are not all created the same:
- Full-fat Dairy
- Animal products (such as eggs)
- Fermented animal products
For those with IBD, pasteurized and aged dairy, such as cheeses (like Swiss, Provolone, Gouda, Cheddar, Edam, Gruyere) or fermented dairy products (such as plain yogurt) may be better tolerated, given they are lower in lactose. These products also offer gut-enriching microbes through the fermentation process.
My Take on Dairy, Animal Byproducts and IBD
Lean meats, aged cheeses, and fermented dairy products can be excellent options for people with IBD that help contribute to overall dietary fat intake. For the average IBD patient, choose fermented or aged dairy for the gut microbiome benefits and full-fat, plain instead of sweetened. The fat content will keep you satisfied (so you do not need to consume as much at a sitting). If able, choose grass-fed or pasture raised sources to increase your omega-3 intake as well as other vitamins and minerals that are more abundant in these sources.
Be sure to discuss animal/fat options with your dietitian if you have further concerns around dietary fat intake in your particular case. A dietitian may recommend full-fat products for satiety or weight gain or low-fat options if indicated.
There are many different dietary approaches, such as the Mediterranean Food Diet for general healthy eating steps, that emphasize healthy fats and whole foods. Your dietitian and GI team can help you to find the approach to IBD treatment that is right for you personally. For more information on whole foods and IBD, download my 4 page handout “Nutrition for Kids and IBD” here.
Fat, Flares, and Symptom Management
During a time of “flare” in IBD, there may be certain types of fats you want to avoid. Generally, a gut-specialized dietitian can help you find what fatty foods trigger symptoms. Fats can and should be maintained in the diet during periods of inflammation, and adjustments to promote tolerance can be made.
6 Tips for Consuming IBD-Friendly Fats & Managing Symptoms during a Flare
There are three main parties to have on board when making sure your diet is full of healthy fats —you, your support system, and your healthcare team. Making sure everyone is on the same page can provide you the support you need to make small but meaningful shifts towards a healthier diet each day.
Here are some tips for consuming fats for health, satiety and symptom management:
- Add a little fat with each meal and snack – this also improves the taste and texture of your food.
- Try small portions more often, rather than larger, fatty meals.
- Modify the consistency of the fat to increase the tolerability of that food for you. For example, choose nut butters instead of whole nuts if you need to.
- Talk to a dietitian who can help you adjust your tolerance of fat-containing foods during a flare or for cases such as stricturing disease or if you have an ostomy.
- Pair fats with fruits or veggies to make them more appealing.
- Listen to your body’s cues for fullness while experimenting with healthy fats.
Pulling it Together: The Take-Home Messages for Fat, Colitis and IBD
While we are learning a lot about fat and inflammation, we still have A LOT to look into. Besides the Standard American Diet, other environmental factors such as obesity, sleep, physical activity/inactivity and others play a role in IBD management. With that being said, there are areas to focus on when it comes to fat intake with what we know in 2022:
⭐ UNSATURATED FATS
MUFAs and Oils–
Oils are meant for different uses, include daily:
- Cooking– Use virgin or pure olive oil often, and sesame oil, sunflower oil, safflower oil, or peanut oil when you want variety!
- Sauteing– avocado (my favorite), canola and peanut oils
- Baking– avocado, canola oil, almond oil, grapeseed oil, coconut oil (less often for UC)
- Other (i.e. salad dressing, finishing oil)- Virgin/pure olive oil, avocado oil (mild in flavor), flaxseed oil (stronger in flavor)
MUFAs & Nuts/Seeds–
If you enjoy them, it is okay to incorporate nuts and seeds daily as a snack or to enhance the taste and texture of a meal as tolerated. You still reap the nutritional benefits if you need to consume these as a nut or seed butter to improve tolerance.
- Tofu (bean) that contains MUFAs
- Almonds
- Walnuts
- Cashews
- Pecans
- Macadamias
- Sunflower seeds
- Pumpkin seeds
- Flaxseed
- Chia seed
- Hemp seeds
PUFAs–
Include n-3 sources in the diet from fish weekly
- UC/CD – Wild caught fish (Ex: Salmon, Mackerel, Herring, Sardines) vs. farm raised as much as able
- Tofu (Choose organic, look for options with the fewest ingredients on the food label)
⭐ SATURATED FATS
Red Meat–
- UC – Prudent to REDUCE intake per the IOIBD recommendations. With this in mind it is IMPORTANT TO REPLACE and focus on other sources of fats (noted above) and whole foods.
- UC/CD – Think of the quality of meat and source. Try to consume grass-fed beef and poultry sources most of the time which will decrease intake of Myristic Acid subsequently as well and improve the ratio of n6:3.
Processed and Cured Meats–
- UC/CD – Limit or avoid
Trans Fats– Avoid
⭐ DAIRY & ANIMAL BYPRODUCTS
As tolerated–
- Prioritize fermented dairy such as aged cheese, plain yogurt (no sugars or additives), plain Kefir
- Prioritize grass-fed sources of fermented dairy when/if able
Kim’s Evidence-Based Fat Guide Pyramid
Referencing the image below, you can find what fats are right for you and plan your diet accordingly. It may require some modification, for example if you avoid meat, or follow more of a plant-based diet.
Fresh chicken breast and eggs are considered a mandatory food on the Crohn’s Disease Exclusion Diet (CDED). Working with a dietitian can help you to determine what forms of fat are appropriate for your diet and health.
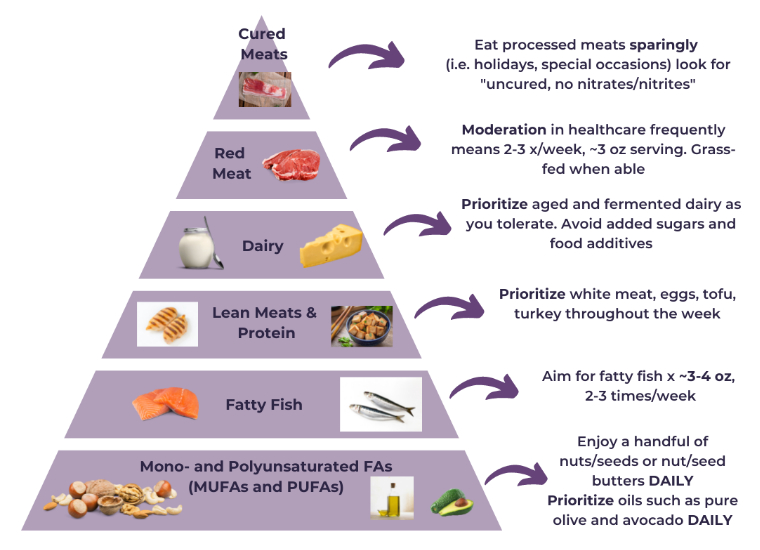
The Final Word On Fat in IBD
As you can see, fats are far more complex than the media gives them credit for. They are also necessary. The goal is not to eliminate what you love, but to prioritize those fats highlighted above and select others less often. Don’t forget to ENJOY your food as you eat it.
When it comes to fat you’ll find what forms of fat work for your IBD and food preferences. In general, avoiding highly-processed meats, and trans fats is suggested. If you haven’t ventured out lately, I challenge you to try some of the new fat sources above like new oils, nut or seed butters or maybe some canned sardines in Caesar salad dressing!
Don’t forget — as a dietitian, I can help you navigate finding fat-friendly IBD foods and more.
References
- Open Oregon. Classification of Nutrients. OpenOregon.pressbooks.pub. Accessed 2022.
- Sasson AN, Ingram RJM, Zhang Z, Taylor LM, Ananthakrishnan AN, et al. The role of precision nutrition in the modulation of microbial composition and function in people with inflammatory bowel disease. Lancet Gastroenterol Hepatol. 2021;6(9):754-769.
- Watson S. How A Registered Dietitian Can Help You With Cholesterol. Alittlenutrition.com. Published June 2021.
- Gropper SS, Smith JL, Carr TP. Advanced Nutrition and Human Metabolism. 7th ed. Wadsworth Publishing; 2018.
- Levine A, Rhodes JM, Lindsay JO, Abreu MT, Kamm MA, et al. Dietary Guidance From the International Organization for the Study of Inflammatory Bowel Diseases. Clin Gastroenterol Hepatol. 2020;18(6):1381-1392.
- Barnes EL, Nestor M, Onyewadume L, de Silva PS, Korzenik JR, et al. High Dietary Intake of Specific Fatty Acids Increases Risk of Flares in Patients With Ulcerative Colitis in Remission During Treatment With Aminosalicylates. Clin Gastroenterol Hepatol. 2017;1(9):1390-1396.
- Fritsch J, Garces L, Quintero MA, Pignac-Kobinger J, Santander AM, et al. Low-Fat, High-Fiber Diet Reduces Markers of Inflammation and Dysbiosis and Improves Quality of Life in Patients With Ulcerative Colitis. Clin Gastroenterol Hepatol. 2021;19(6):1189-1199.
- Nguyen LH, Cao Y, Hur J, et al. The Sulfur Microbial Diet Is Associated With Increased Risk of Early-Onset Colorectal Cancer Precursors. Gastroenterology. 2021;161:1423-1432.
- Olendzki B, Bucci V, Cawley C, Maserati R, McManus M, et al. Dietary manipulation of the gut microbiome in inflammatory bowel disease patients: Pilot study. Gut Microbes. 2022;14(1).
- Rizzello F, Spisni E, Giovanardi E, Imbesi V, Salice M, et al. Implications of the Westernized Diet in the Onset and Progression of IBD. Nutrients. 2019;11(5):1033.
- Zagarella C. 10 Best Cooking Oils With. Bistromd.com. Published 2020.

Hi! I'm Kim Braly, RD, a clinical researcher and IBD Nutrition Consultant. I specialize in cutting-edge dietary therapies for inflammatory bowel disease that have been shown in multicenter trials to decrease inflammation, alleviate IBD symptoms and induce remission. I'm passionate about offering this effective new option to patients and their families with my 3D-Dietary™ Approach for IBD and helping to usher in a new era of IBD treatment through mentoring and research trial consultation. Let's see what diet can do for you.
ABOUT
FOR PATIENTS

Flares Happen!
You can't always put your life on hold when IBD rears its head, but you can make this your easiest flare yet. My proven diet and lifestyle tips support your gut, body, mind & emotions for a faster recovery and a longer remission.
FOR PARENTS

Is Your Child’s Weight Dropping Fast?
You don't have to stand helpless during an IBD flare. Feed your child foods proven to minimize triggers, calm inflammation, and repair the gut. Get them healing and growing!




